



Looking kind of empty in here.
We recommend:

Get advanced insights into symptoms, fertility, and other health outcomes. Prelim results in 1-3 days.

Discover the best BV medication options to treat bacterial vaginosis. Learn about pharmaceutical treatments and understand your vaginal microbiome.
Words by Caitlyn Tivy, DPT, OCS
Scientifically edited by Dr. Krystal Thomas-White, PhD
Medically reviewed by Dr. Kate Stewart, MD
Whether you just received a diagnosis of bacterial vaginosis (BV) or have struggled with recurrent bouts of BV for ages, you’re likely on the hunt for a fix.
Bacterial vaginosis is a vaginal infection caused by an imbalance in the bacteria that make up your vaginal microbiome. Essentially, healthy vaginal bacteria are replaced by disruptive “bad” bacteria, creating an infection.
“Okay, easy”, you may be thinking. “I just need to kill off the bad bacteria and everything will go back to normal!”
Unfortunately, it’s not quite that simple. With the many bacterial vaginosis treatment options on the market, it’s hard to know what will help: will this new medication or that new supplement shift your vaginal microbiome to a healthier, protective state, or will it keep you stuck in the endless cycle of having bacterial vaginosis over and over again?
Read on to learn about BV medication, including the most common pharmaceutical treatments for bacterial vaginosis and how they affect your vaginal health.
Before we dive into the treatment options, it's important to understand what causes bacterial vaginosis.
Bacterial vaginosis is a common vaginal infection caused by an imbalance of bacteria in the vagina. Normally, the vagina contains a healthy balance of different types of bacteria, with Lactobacilli being the most dominant.
BV occurs when there is a decrease in Lactobacilli and an overgrowth of harmful bacteria, such as Gardnerella and Prevotella. This imbalance disrupts the vaginal pH, leading to symptoms such as abnormal vaginal discharge that may be thin, grayish-white, and have a strong fishy odor. Many women don't experience any bacterial vaginosis symptoms.
Bacterial vaginosis isn't considered a sexually transmitted infection (STI), but it's more common if you're sexually active. Having unprotected sex, multiple sex partners, or a new sex partner makes you more likely to develop BV. Other behaviors, such as smoking or douching, can put you at an increased risk of developing bacterial vaginosis.
It's important to consult a healthcare provider for proper BV diagnosis and treatment if you suspect you have an infection. Treatment usually involves prescription antibiotics to restore the natural balance of bacteria in the vagina and alleviate uncomfortable symptoms. Below, we take a look at the available treatment options for bacterial vaginosis.

Recurrent symptoms? Get Evvy's at-home vaginal microbiome test, designed by leading OB-GYNs.
If you've been diagnosed with BV, you're not without options. The main treatments include antibiotics like metronidazole and clindamycin, which work to rebalance the vaginal microbiome by targeting the overgrowth of pathogenic bacteria. There’s also boric acid, a well-known supplement often used in cases of recurrent bacterial vaginosis.
Each treatment option works a little differently, and your healthcare provider can help determine the best fit for your body and lifestyle. Read on to learn more about how these medications work, how they're used, and what to know before starting treatment.
Brand name: Flagyl®
Type of medication: antibiotic
Class: nitroimidazoles
Administration route: oral (pills taken by mouth) or intravaginal (gel applied internally)
Antibiotic medications are commonly prescribed to treat bacterial infections, and bacterial vaginosis is no exception. Metronidazole is an antibiotic used to kill anaerobic bacteria (bacteria that don’t require oxygen to survive) and other microbes that can cause infections.
It’s been tested and found to be effective against several bacterial species that are associated with bacterial vaginosis, including:
No antibiotic medication can always wipe out every bacterial species at once. Some BV-related bacteria are resistant to metronidazole (i.e., metronidazole won’t kill them), including:
However, there’s some good news: Lactobacilli species, the “good” bacteria that are the most common in healthy vaginas, are also resistant to metronidazole. This means that treatment with metronidazole will get rid of the disruptive, or “bad” bacteria while sparing your healthy Lactobacilli.
Guidelines by the Centers for Disease Control and Prevention (CDC) currently recommend that metronidazole be given either orally (as pills) or via intravaginal administration to treat BV. If your healthcare provider prescribes metronidazole for your BV, they may recommend one of the following courses:
While these are common recommendations, recall that your healthcare provider must take your unique medical history and sensitivities into account when determining the correct treatment regimen for you.
Brand name: Cleocin®
Type of medication: antibiotic
Class: lincomycins
Administration route: oral (pills taken by mouth) or intravaginal (tablets inserted or cream applied internally)
Clindamycin is another antibiotic commonly used to treat BV. It works by slowing and sometimes stopping the growth of bacteria. Similar to metronidazole, clindamycin is effective against several bacterial species that can cause bacterial vaginosis, including:
Despite this list, clindamycin isn’t a silver bullet against BV-related bacteria. For example, it is not as effective against Prevotella species that can contribute to bacterial vaginosis. Clindamycin can also kill off the protective (Lactobacilli) bacteria along with the disruptive bacteria, which may contribute to bacterial vaginosis coming back again later.
Both vaginal and oral clindamycin should be taken for seven days. Alternatively, your provider may recommend using clindamycin “ovules”, which are basically little pills you place inside the vagina and allow to dissolve. Ovule treatment takes just three days.
Brand name: Tindamax®
Type of medication: antibiotic + antiprotozoal
Class: nitroimidazole
Administration route: oral (pills taken by mouth)
Tinidazole is an antibiotic that can kill protozoa (microscopic single-celled animals). It belongs to the same class of antibiotics as metronidazole and is also effective against many of the bacteria involved in bacterial vaginosis.
Tinidazole can kill Gardnerella vaginalis, a bacterial strain commonly associated with bacterial vaginosis.
However, less is known about how well it works against other specific BV-related species. As the research on BV treatment progresses, we may learn that tinidazole can also act against other problematic bacterial strains.
Like metronidazole, tinidazole does not kill Lactobacilli, the protective bacteria of a healthy vaginal tract. Researchers have also shown that it may cause fewer negative side effects on the GI tract, making it an attractive alternative to metronidazole in some cases.
To treat bacterial vaginosis, your provider may prescribe tinidazole to be taken orally for two or five-day courses. Though less convenient, longer courses of treatment appear to be more effective against bacterial vaginosis than shorter ones.
Brand name: Solosec®
Type of medication: antibiotic
Class: nitroimidazole
Administration route: oral (granules taken by mouth)
Secnidazole is an antibiotic in the same class as metronidazole and tinidazole, and it, too, works by stopping bacterial growth. However, unlike its cousins, it’s typically taken orally in a single dose.
Secnidazole is effective (and ineffective) against similar sets of bacterial species as metronidazole and tinidazole. It also spares the beneficial Lactobacilli strains that help maintain vaginal health.
This medication comes in the form of granules you sprinkle on soft food like yogurt to ingest. Typically, only one dose of these granules is required to treat bacterial vaginosis.
The only non-prescription option on this list, boric acid is a white powder made from borax, a naturally occurring mineral. It’s composed of the elements boron, hydrogen, and oxygen.
Boric acid has antimicrobial and antifungal properties, suggesting that it may be a useful addition to the treatment regimen for people with recurring BV. It hasn’t been studied as much as the medications we’ve discussed, so we don’t have a reliable breakdown of the BV-related bacterial species it can and can’t impact.
FYI, generally, boric acid prescribed by a doctor tends to be more pure and less likely to cause adverse reactions than boric acid purchased OTC or online. So if you're going to use boric acid, always try to get it prescribed by a healthcare provider.
As we’ve discussed, the initial treatment timeframes for the various bacterial vaginosis medications vary, though most can be completed in a week or less. It’s important to complete the entire treatment you’re prescribed for bacterial vaginosis, even if your symptoms go away before you complete it. This is one way to help prevent bacterial vaginosis from coming back.
Unfortunately, up to 50% of people who are diagnosed with BV will experience a recurrence within one year.
If your BV symptoms return after an initial round of treatment, it’s important to consult with your medical provider. If this is the first time your BV has recurred, or if the first round of treatment simply didn’t work, they may recommend a second round of the same course of medication.
However, if your bacterial vaginosis keeps coming back, it’s typically time to try an alternative medication and administration route (i.e., an intravaginal gel instead of oral pills).
While additional rounds of pharmaceutical treatment can be effective in knocking out stubborn BV, they often require much longer courses lasting several weeks or months. Additionally, the protection these medications provide often disappears when you stop taking them, and the bacterial vaginosis can come right back, again.
Yes, boric acid and clindamycin can be used together, but timing is key. Clindamycin is a prescription antibiotic that treats BV by targeting anaerobic bacteria, while boric acid helps maintain vaginal pH and prevent recurrence. Using them at the same time (especially both vaginally) can cause irritation or reduce the effectiveness of one or both.
For best results, take one before the other (our clinicians often recommend doing the boric acid first). Some providers may recommend a short waiting period (24–48 hours) between finishing one and starting the other.
Always check with your healthcare provider before combining treatments, especially if you're using prescription medications. The goal is to treat the infection effectively while giving your microbiome the best chance to recover and thrive.
Boric acid and metronidazole can be used in the same treatment journey, but they shouldn’t typically be used at the same time. Metronidazole is a first-line antibiotic for BV and can be taken orally or used vaginally. If you use boric acid vaginally at the same time, it may reduce the antibiotic's effectiveness or increase the risk of irritation.
Like clindamycin, forbest results, take one before the other (our clinicians often recommend doing the boric acid first). This protocol can be especially helpful for people who experience frequent BV flare-ups. If you're unsure how to time these treatments or have ongoing symptoms, talk to your provider. Personalized protocols are often the most effective, especially when working toward long-term microbiome balance.
Managing BV often involves a combination of prescription treatments and over-the-counter (OTC) support to help restore and maintain vaginal health. First-line medications like metronidazole and clindamycin are prescribed to clear the infection.
For those dealing with recurrent BV or looking to support their vaginal microbiome after treatment, options like boric acid suppositories and probiotics can play a helpful role. Here’s a breakdown of common products used in a BV care plan:
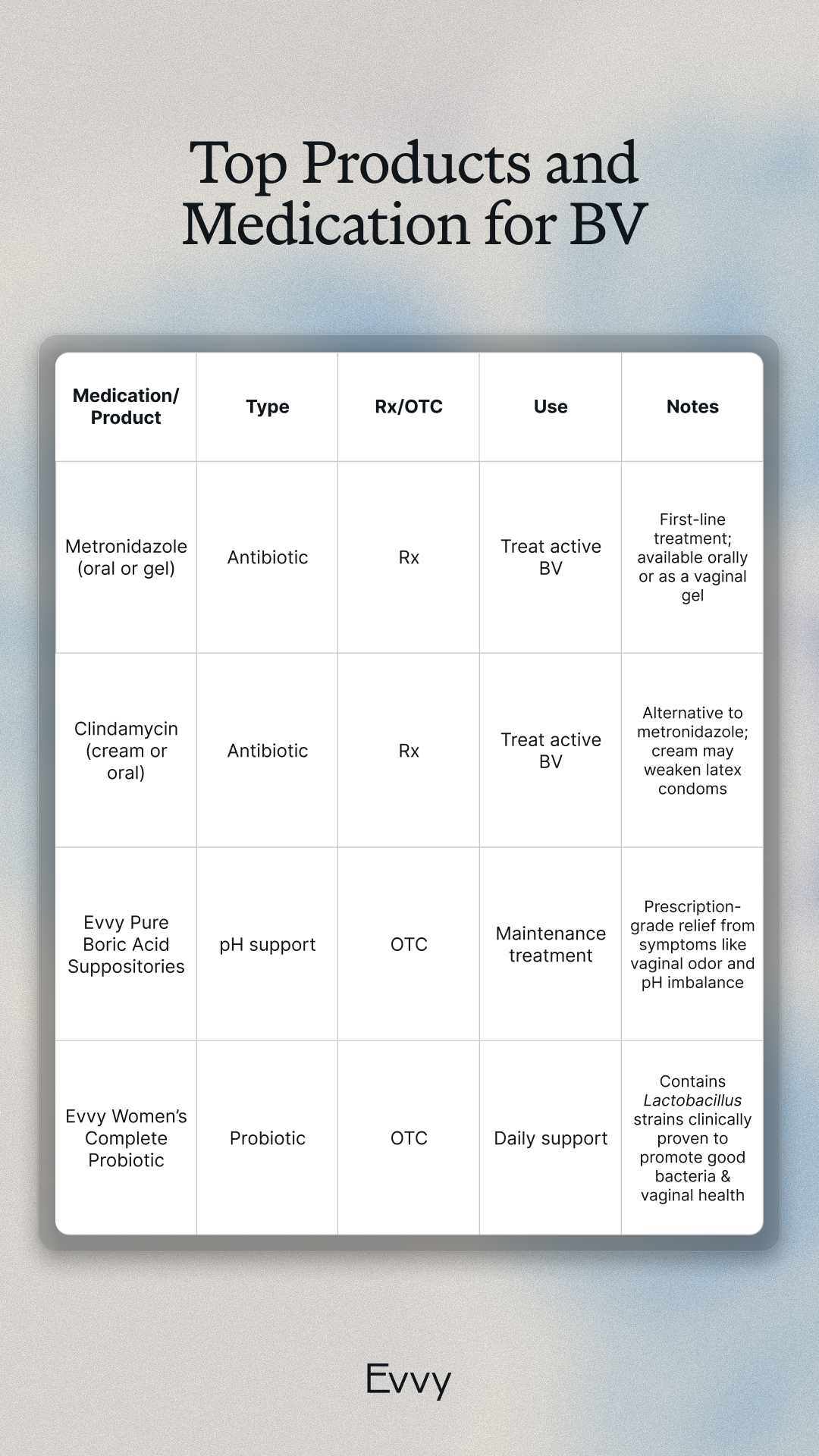
Antibiotics target the immediate infection, while products like boric acid and probiotics can help support ongoing microbiome balance. For the best results (especially if you deal with frequent BV), talk to your provider about creating a personalized plan that combines treatment with preventative care.
Eligible Evvy users can access a personalized prescription treatment plan developed by a licensed provider, based on the results of their Evvy Vaginal Health Test — all from the comfort of home. This approach allows for targeted, data-backed care that supports both immediate relief and long-term vaginal health.
What’s a person with BV to do? First things first: if you’re struggling with stubborn, recurrent bacterial vaginosis, take a deep breath and know you’re in the right place. Evvy is working to break down barriers in our understanding of the vaginal microbiome and its role in recurrent BV.
Whether or not you have bacterial vaginosis, taking an Evvy Vaginal Health Test can help you better understand the makeup of your vaginal microbiome. Specifically, whether it’s dominated by bacteria associated with BV, and if so, which types. If your results indicate potential signs of BV, a licensed provider will review your test and, if appropriate, diagnose bacterial vaginosis. From there, they can create a personalized treatment plan (including prescription antibiotics) based on your unique microbiome, symptoms, and health history.
With an Evvy Membership, you can easily monitor changes in your microbiome and track your body’s response to different treatment regimes. Knowledge is power: the better you understand your unique microbiome, the more accurately you can tailor your care to keep it healthy.
We know that searching for effective care for vaginal symptoms can be overwhelming. We’re here to provide you with up-to-date research on treatments and personalize your care so you feel supported at every step.
The first-line treatment for bacterial vaginosis is antibiotics like metronidazole or clindamycin. These can be taken as pills you take by mouth or a vaginal cream. Your doctor will decide which option is best based on how severe your BV symptoms are and your medical history. It's super important to follow their advice closely and finish the entire course of medication, even if you start feeling better sooner. This ensures that the infection is completely cleared and lowers the likelihood of it coming back.
Sometimes, especially if it's a mild case and not causing noticeable symptoms. But here's the thing: even if the symptoms seem to get better on their own, the imbalance of bacteria in your vagina might still be there, so we wouldn't recommend chancing it. Untreated BV can lead to recurrent infections and other health problems, including pelvic inflammatory disease (PID), pregnancy complications (such as preterm birth or low birth weight), and a higher risk of sexually transmitted infections. So, if you're noticing any signs like unusual vaginal discharge or vaginal odor, it's a good idea to chat with your healthcare provider.
The fastest way to clear up bacterial vaginosis is typically with a prescription antibiotic, such as metronidazole or clindamycin, which are considered first-line treatments. These medications work by targeting the overgrowth of disruptive bacteria in the vaginal microbiome and can usually start relieving symptoms within a few days. Oral or vaginal forms are available, and your healthcare provider will recommend the best option based on your symptoms and medical history. It’s important to complete the full course of antibiotics, even if symptoms improve early, to ensure the infection is fully treated. After finishing treatment, many people choose to use boric acid suppositories to help restore vaginal pH and reduce the chance of recurrence. While antibiotics are the fastest and most effective treatment, addressing underlying imbalances in the vaginal microbiome (through supportive care like probiotics) can help prevent future flare-ups and support long-term vaginal health.
The best boric acid for supporting vaginal health (especially after a BV treatment) is one that’s pure, clinically backed, and designed specifically for vaginal use. Evvy Pure Boric Acid Suppositories are made with 600 mg of prescription-grade boric acid and are free from unnecessary fillers, dyes, or fragrances. While boric acid doesn’t treat the infection itself (it’s not a replacement for antibiotics), it can be incredibly helpful in restoring pH balance and preventing recurrent BV when used after completing antibiotic treatment. When choosing a boric acid product, look for those that are third-party tested for purity and safety, and come in pre-filled capsules for ease of use and proper dosage. It's always best to use boric acid under the guidance of a healthcare provider, especially if you’re managing recurrent BV or combining it with other treatments.