



Looking kind of empty in here.
We recommend:

Get advanced insights into symptoms, fertility, and other health outcomes. Prelim results in 1-3 days.

Learn about UTIs in women: symptoms, causes, risk factors, treatment options, prevention tips, and when to see a doctor.
Words by Olivia Cassano
Scientifically edited by Dr. Krystal Thomas-White, PhD
Medically reviewed by Dr. Kate McLean MD, MPH, FACOG
A urinary tract infection (UTI) is one of the most common infections people with a vagina experience. In fact, about half of women will have at least one UTI in their lifetime, and many will have more than one. While UTIs are common, they can be uncomfortable and sometimes difficult to recognize, especially because their symptoms can overlap with other vaginal or urinary conditions.
UTIs occur when bacteria enter the urinary tract and overgrow. This can cause symptoms like burning when you pee, frequent urination, pelvic pressure, or cloudy urine. In some cases, the infection can spread beyond the bladder and affect the kidneys, which is more serious.
The good news is that most urinary tract infections are treatable, especially when caught early. Understanding what causes UTIs, what symptoms to watch for, and how they’re diagnosed can help you get the right care quickly.
Keep reading for the 101 on what a UTI is, the different types, common symptoms, risk factors, and how Evvy’s UTI+ Test can help identify the exact microbes involved so you can get the most effective treatment.
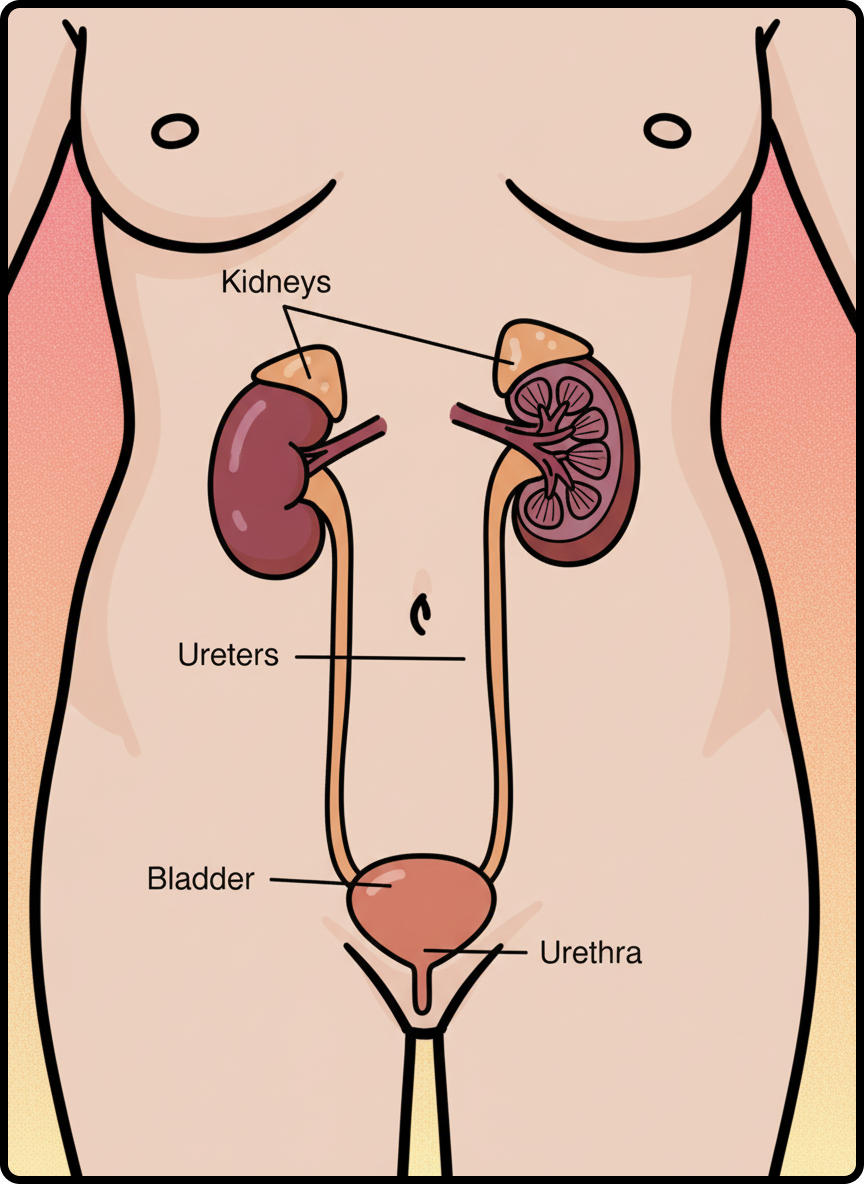
A urinary tract infection is — as the name suggests — a bacterial infection that occurs anywhere in the urinary system, which consists of several interconnected organs that work together to produce and flush urine from the body. The urinary tract includes the kidneys, ureters, bladder, and urethra.
The kidneys filter waste and excess fluid from your blood to create urine. Urine then travels through thin tubes called ureters into the bladder, where it’s stored until you pee. Finally, urine exits the body through the urethra, the tube that carries urine out of your bladder.
Urinary tract infections happen when bacteria enter the urinary tract (usually through the urethra) and begin multiplying. Most infections start in the lower urinary tract, which includes the urethra and bladder. If the infection spreads upward, it can reach the kidneys, which is more serious and requires prompt medical care.
There are three main types of UTIs based on where the infection occurs:
While all three are considered UTIs, they can cause slightly different symptoms and require different levels of medical attention. The majority of UTIs are bladder infections, which are uncomfortable but usually pretty straightforward to treat.
Cystitis is the most common type of urinary tract infection. It occurs when bacteria infect the bladder, the organ that stores urine before it leaves the body.
Most bladder infections are caused by bacteria that normally live in the digestive tract, especially Escherichia coli (E. coli). These bacteria can enter the urethra and travel up into the bladder, where they begin to multiply.
Bladder infections often cause the classic UTI symptoms many people recognize:
Although cystitis can be painful and disruptive, it’s usually not dangerous if treated on time. Antibiotics typically clear the infection within a few days. However, if a bladder infection goes untreated, the bacteria can spread to the kidneys and cause a more serious infection.
A kidney infection, also called pyelonephritis, happens when bacteria travel from the bladder up through the ureters and infect one or both kidneys.
This type of urinary tract infection is less common but more serious. The kidneys play an essential role in filtering waste from the blood, so an infection there can allow bacteria to enter the bloodstream, which can be life-threatening.
Symptoms of a kidney infection often include:
These symptoms usually appear alongside typical UTI symptoms like painful urination or urgency. It's really important to get medical help for kidney infections right away. Typically, antibiotics can help treat these infections, and sometimes, a hospital stay might be necessary. To keep things from getting worse, it's best to tackle bladder infections early on. Promptly treating them can help prevent them from spreading to the kidneys.

Recurrent symptoms? Get Evvy's at-home vaginal microbiome test, designed by leading OB-GYNs.
UTI symptoms can vary depending on which part of the urinary tract is infected. Lower urinary tract infections, such as bladder infections, tend to cause urinary symptoms. Infections that spread to the kidneys often cause more systemic symptoms, like fever or nausea. Symptoms can look different in older people, who may experience confusion, fatigue, or general discomfort instead of typical urinary symptoms.
Lower urinary tract infections (UTIs) are common and affect the urethra and bladder. If you’ve ever experienced one, you know they usually come with some uncomfortable symptoms related to urination and bladder discomfort.
One of the most noticeable signs is a burning or stinging sensation when you pee. This happens because the lining of your urethra and bladder gets irritated during the infection.
You may also feel like you need to rush to the bathroom all the time. It’s frustrating, especially when it feels like you can’t fully empty your bladder.
Many people also report feeling pelvic pressure or discomfort in the lower abdomen, as if the bladder is never quite empty.
Another common symptom is changes in your urine. It might look cloudy or darker than usual and sometimes have a stronger or unusual smell. In some cases, you might even notice a hint of pink or reddish tint, which is a sign that blood is present in your urine.
If you’re experiencing these symptoms, it’s always a good idea to reach out to a healthcare professional for advice. Urinary tract infections aren’t generally serious, as long as you treat them ASAP.
When a urinary tract infection spreads to the kidneys, symptoms usually become more severe and affect the whole body.
A fever is one of the most common signs of a kidney infection, often accompanied by chills or sweating. Many people also feel nauseous or may vomit.
Another key symptom is back or side pain, usually just below the ribs. This flank pain often occurs on one side of the body and can be quite uncomfortable.
Because kidney infections can become serious quickly, symptoms like fever, back pain, and nausea, along with urinary symptoms, should prompt medical attention right away.
Urinary tract infections happen when bacteria enter the urinary tract and begin to multiply. In most cases, these bacteria come from the digestive tract. The most common culprit is E. coli, a bacterium that normally lives in the intestines but can cause infection if it reaches the urinary tract.
Bacteria usually enter through the urethra and travel upward into the bladder. This can happen during everyday activities like sex, wiping after using the bathroom, or normal movement that transfers bacteria from the surrounding skin.
Once inside the urinary tract, bacteria can multiply if the body’s natural defenses don’t fight them off or flush them out quickly.
Urinary tract infections are significantly more common in women than in men, mainly because of female anatomy, hormonal changes, and certain everyday behaviors that make it easier for bacteria to reach and grow in the urinary tract. Around 50–60% of women will experience at least one in their lifetime, and many will have recurrent UTIs.
Anatomy plays the biggest role. Women are more prone to UTIs because their urethra is shorter and located closer to the rectum. This means bacteria — most often E. coli from the gut — have a shorter distance to travel to reach the bladder. Because of this, everyday activities like using the bathroom, wiping, or having sex can move bacteria toward the urinary tract.
Hormones also affect your risk of UTIs throughout your life. During pregnancy and the postpartum period, hormonal and physical changes can slow urine flow and alter the urinary tract, making infections more likely. Around menopause, declining estrogen levels can thin and dry the tissues of the vagina and urethra and change the balance of protective vaginal bacteria. These changes weaken natural defenses against infection, including UTIs.
Research also shows that bacteria from the vaginal microbiome can sometimes move into the bladder and contribute to urinary tract infections, especially recurrent ones. When the balance of microbes in the vagina shifts, certain bacteria may be more likely to colonize the urinary tract, leading to recurrent infections. Because the vaginal and urinary microbiomes are closely connected, understanding which microbes are present can be helpful when UTIs keep coming back. Evvy’s UTI+ Test is designed to detect a broad range of UTI-associated bacteria using PCR-based technology, helping identify the microbes that may be contributing to persistent or recurrent symptoms.
You might have heard that wiping from back to front after using the bathroom could increase your risk of getting a urinary tract infection. The reason is that it could potentially move bacteria from the anus toward the urethra.
It makes sense when you think about it: most UTI-causing bacteria come from the digestive tract. So, if those bacteria get too close to the urethral opening, it might increase the risk of them entering the urinary tract.
But here’s the thing: research on this topic has shown mixed results. Some data suggest that the direction you wipe might not have a huge impact on UTI risk, while others do support the typical recommendation to wipe from front to back (especially in postmenopausal women).
Even though the evidence isn’t crystal clear, most healthcare providers still suggest the front-to-back method. It’s a simple habit that could help minimize the transfer of bacteria and promote better urinary and vaginal health.
While bacterial growth is the direct cause of urinary tract infections, several factors can increase the likelihood that bacteria enter the urinary tract or multiply once they’re there. These include lifestyle habits, certain types of birth control, and underlying medical conditions.
Common UTI risk factors include:
UTI symptoms can feel pretty distinctive, but they’re not always unique to UTIs. Other conditions, including yeast infections, bacterial vaginosis (BV), and some sexually transmitted infections (STIs), can cause similar symptoms, such as burning, irritation, or discomfort when you pee. Because of this overlap, testing is the best way to confirm whether you actually have a UTI.
At-home UTI tests can be a helpful first step if you’re experiencing symptoms, but clinic testing is still the gold standard for diagnosing and treating urinary tract infections.
Most over-the-counter UTI test strips work by detecting chemical markers in urine, such as white blood cells and nitrites, which can indicate that an infection may be present. When used correctly and in combination with symptoms, these tests can provide quick results and help you decide whether to contact a healthcare provider.
However, test strips have limitations. They can sometimes miss infections — for example, if the bacteria causing the infection don’t produce nitrites, if the infection is in its early stages, or if factors like vitamin C, medications, or improper sample collection interfere with the results. They also can’t identify the specific bacteria responsible for the infection.
Clinic testing provides a more complete picture. In a medical setting, clinicians typically combine your symptoms with a urine dipstick, microscopic urinalysis, and, sometimes, a urine culture to identify the organism causing the infection and determine which antibiotics may work best.
Some newer at-home tests use more advanced technology. For example, Evvy’s UTI+ Test uses PCR-based molecular testing to analyze microbial DNA in your urine. Instead of just looking for general signs of infection, it identifies specific microbes commonly associated with urinary tract infections. By detecting these pathogens at the DNA level, Evvy’s test can pick up infections that standard dipstick tests — and sometimes even traditional urine cultures — may miss. This more detailed view can be especially helpful for people experiencing persistent or recurrent symptoms, helping identify potential causes and support more informed conversations with a provider about treatment options.
Urinary tract infections are usually treated with a short course of antibiotics along with at-home or over-the-counter remedies to ease symptoms. Most people start feeling better within a couple of days. However, it’s important to finish all antibiotics to completely clear the infection and reduce the risk of recurrence or antibiotic resistance.
If you're dealing with a straightforward bladder infection and you're generally healthy, doctors typically recommend a short course of antibiotics, usually lasting 3 to 5 days, though it can go up to 7 days depending on the medication and local practices. Some common options include trimethoprim-sulfamethoxazole (Bactrim), nitrofurantoin (Macrobid), or ciprofloxacin (Cipro). The choice of antibiotic will take into account factors such as your health history, whether you’re pregnant, the severity of your symptoms, local resistance patterns, and, sometimes, the results of a urine culture.
If symptoms don’t improve after a couple of days or worsen, you should contact your provider, as a different antibiotic or additional testing may be needed.
To help ease discomfort while your body fights a urinary tract infection, the following at-home and over-the-counter remedies can be used alongside prescribed antibiotics:
Using these remedies alongside a full course of prescribed antibiotics can help reduce discomfort and support a faster recovery from a urinary tract infection.
While it’s not always possible to completely prevent UTIs, certain habits and lifestyle choices can significantly reduce your risk of infection. Key strategies include:
Incorporating these habits won’t prevent urinary tract infections entirely, but it can lower the likelihood of developing a UTI and support overall urinary and vaginal health.
You should contact your provider if you start experiencing any classic symptoms of a UTI. Urinary tract infections are pretty easy to treat, but they require prescription antibiotics. Plus, your provider can rule out any other potential cause for your symptoms, including a vaginal infection or STI.
You should also speak to your provider if your symptoms aren’t improving after a couple of days of treatment, or if they seem to be worsening. Persistent symptoms might mean the infection isn’t fully cleared or that something else is going on.
It’s also important to seek immediate help if you have a fever, chills, back or flank pain, vomiting, confusion, or if you’re pregnant, have kidney disease, diabetes, or a weakened immune system, as these could be signs of a kidney infection. Especially during pregnancy, it’s crucial to get prompt care for UTIs, as they can impact both your health and that of your baby if left untreated.
If you find that you’re getting recurrent urinary tract infections, it’s definitely worth discussing it with a provider. Recurring infections might point to underlying factors that can be addressed with tailored prevention strategies.
Urinary tract infections are usually diagnosed based on symptoms and a urine test. A common first step is a urinalysis, which checks the urine for signs of infection, like white blood cells, bacteria, or the presence of nitrites.
If needed, a urine culture may be done. This test allows bacteria in the urine to grow in a lab, so they can be identified and tested for which antibiotics will work best.
For people with frequent or complicated UTIs, doctors might recommend additional tests. Imaging studies, such as ultrasounds or CT scans, can help detect structural issues or kidney stones that may cause recurrent infections.
More advanced molecular testing can also help understand the microbes present and guide more personalized treatment options.
The most common UTI symptoms include a burning sensation when you pee, frequent urges to pee, pelvic pressure, cloudy or strong-smelling urine, and discomfort in the lower abdomen. Some women may also notice blood in the urine. If the infection spreads to the kidneys, symptoms may include fever, chills, nausea, and back pain.
The best way to confirm a urinary tract infection is with a urine test. While symptoms can be suggestive, other conditions can cause similar discomfort. Testing — either in clinic or with an at-home UTI test — can identify whether bacteria are present and help determine the best treatment.
If you suspect you have a urinary tract infection, it’s important not to ignore symptoms or delay treatment, as untreated infections can spread to the kidneys and become more serious. You should also avoid bladder or vaginal irritants, such as scented hygiene products, harsh soaps, or bubble baths, which can worsen discomfort and inflammation. It’s also better to avoid having sex until your infection has cleared, since sex can introduce bacteria into the urethra and may slow down recovery. Holding off on activities that stress or irritate the urinary tract, while following your prescribed antibiotic course, can help you heal faster and reduce the risk of recurrence.
Wiping back to front may increase the chance of transferring bacteria from the anal area toward the urethra. While research on this connection is mixed, most clinicians recommend wiping from front to back as a simple precaution to support urinary health.
When you get the right antibiotic treatment for an uncomplicated urinary tract infection, you'll likely start feeling better within 24 to 48 hours, and you should be back to normal in just a few days. If left untreated, though, the symptoms might stick around longer, and there's a chance the infection could spread to your kidneys. So it's best to address it promptly.
When you have a UTI, your urine may look cloudy or darker than usual, and it may have a strong or unusual smell. Sometimes, even a hint of blood can give your urine a pink, red, or cola color. But remember, just seeing these changes isn’t enough to confirm a UTI; you’ll need tests to get a proper diagnosis.